The first time you see your cat collapse, shake, or stare blankly during a seizure, it hits hard. One second, they are fine, the next, you are frozen, unsure what to do or what it even means.
Watching it unfold can feel helpless and overwhelming. Understanding cat seizure symptoms is the first step in taking back some control.
This blog breaks things down in a way that actually makes sense, from what causes seizures to how they are treated and how they affect your cat’s day-to-day life.
It also covers the three distinct phases every seizure moves through, the difference between focal and generalized episodes, and how to tell a true seizure apart from other conditions that mimic one.
It also tackles the question most people avoid but quietly search for: when to euthanize a cat with seizures, and how to make that call without second-guessing yourself later.
What a Cat Seizure Actually Looks Like?
Not every seizure in cats looks extreme or violent. Some are subtle, while others are hard to miss.
Mild episodes may involve brief staring, twitching, or confusion, whereas severe ones can include a sudden collapse, uncontrolled shaking, drooling, or even loss of bladder control.
Many pet owners first notice something is wrong when their cat seems “absent” or unresponsive.
These moments can last seconds or a few minutes, but feel much longer when you are watching it happen.
Seizures affect roughly 1 to 2% of the feline population, and while they can look terrifying, a single brief seizure is not always a life-threatening emergency, though it always warrants a veterinary evaluation.
The reason it feels so intense is simple: you are witnessing a loss of control in your pet, which triggers panic, even if the episode is short-lived.
Every seizure in cats moves through up to three recognizable phases:
- Pre-ictal phase (aura): This happens minutes to hours before the seizure. Your cat may seem restless, confused, unusually clingy, or may suddenly hide.
- Ictal phase (the seizure itself): This is the active episode, muscle twitching, paddling legs, stiffening, drooling, loss of consciousness, or subtle repetitive behaviors, depending on the type.
- Post-ictal phase (recovery): After the seizure ends, cats often appear disoriented, wobbly, temporarily blind, or unusually aggressive.
Types of Cat Seizures: Focal vs. Generalized
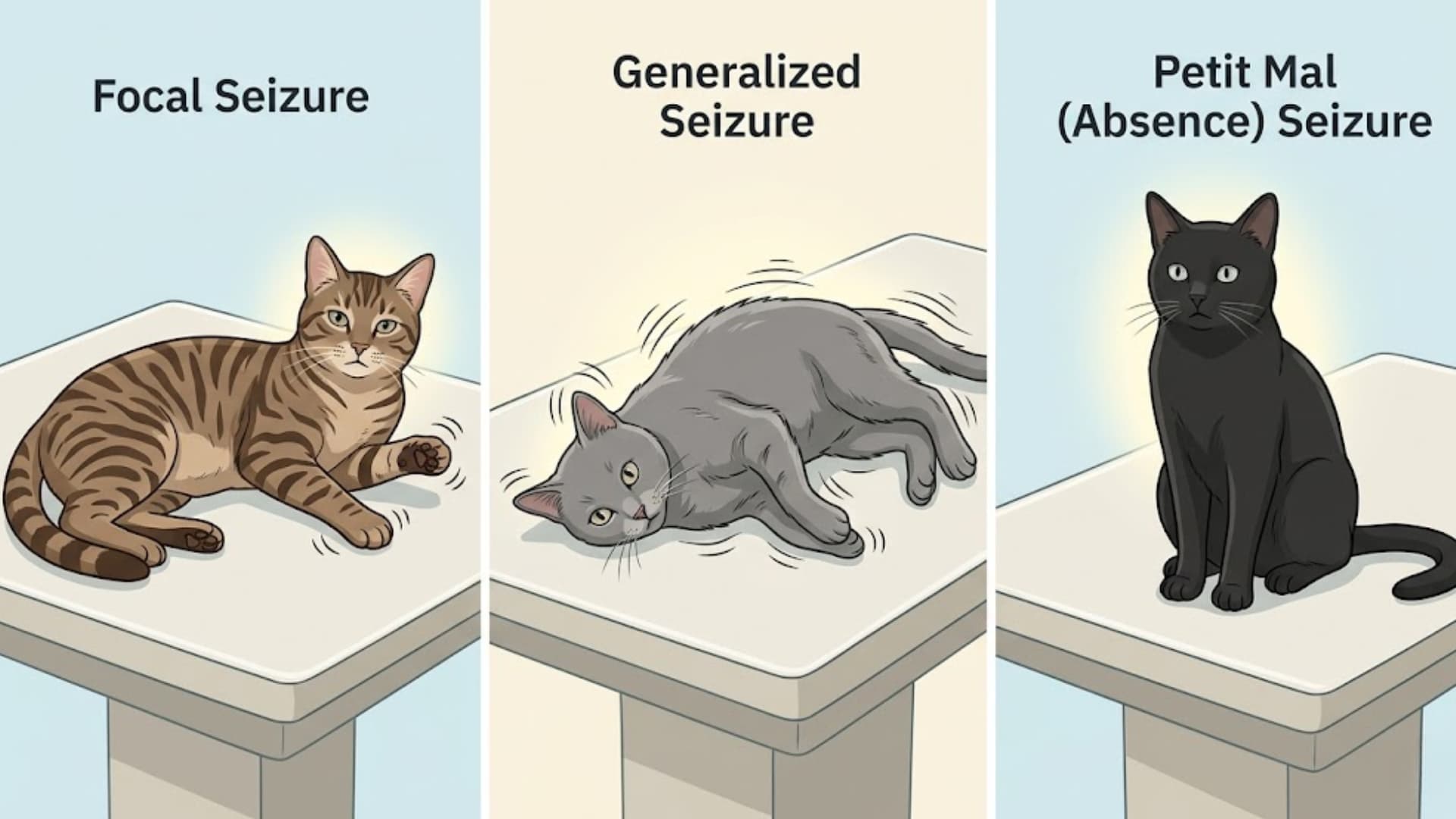
Understanding the type of seizure your cat is having is not just a clinical detail; it directly shapes how your vet diagnoses the cause and selects treatment.
1. Focal (Partial) Seizures
These are actually themost common type of seizure in cats, though they are frequently missed because they look nothing like the dramatic convulsions most people picture.
You might notice one ear twitching repeatedly, a single paw jerking, facial muscle spasms, or repetitive lip-smacking.
A well-known subtype is the “fly-biting” seizure, where the cat suddenly snaps at the air as if chasing invisible insects. Focal seizures can progress into generalized seizures if the electrical disturbance spreads across the brain.
2. Generalized (Grand Mal) Seizures
These involve the entire brain and produce the full-body symptoms most people associate with seizures, loss of consciousness, rigid or paddling limbs, drooling, and loss of bladder or bowel control.
The head is often drawn backward. Grand mal seizures are more dramatic but are actually less common in cats than focal episodes. They typically last 1–2 minutes.
3. Petit Mal Seizures
Less dramatic and frequently overlooked, petit mal seizures do not cause convulsions. Because they are subtle, they are often mistaken for odd behavior or momentary clumsiness.
Instead, your cat may suddenly collapse or stare blankly for a few seconds, then appear completely normal.
Early Cat Seizure Symptoms Most People Miss
Small behavior shifts often show up before seizures, but they are easy to ignore or misread if you do not know what to look for.
- Hiding more than usual: Cats may suddenly withdraw and spend more time under beds or in corners, avoiding interaction without any clear trigger.
- Sudden aggression or fear: A friendly cat may become irritable, hiss, or act scared, reacting to things that normally would not bother them.
- Restlessness or pacing: Repeated walking, circling, or inability to relax can signal discomfort or an accumulation of unusual brain activity.
- Unusual vocalizations: Some cats yowl, whine, or cry out before a seizure in a way that sounds different from their normal meows.
- Excessive attention-seeking: While some cats hide before a seizure, others do the opposite, becoming unusually clingy, following you from room to room, or demanding to be held.
- Vomiting or gastrointestinal upset: Some cats experience nausea, vomiting, or loose stool in the pre-ictal phase — a sign that is easy to dismiss as an unrelated stomach issue.
In my practice in Minnesota, one of the most consistent things cat owners tell me, usually in hindsight, is that their cat had been acting a little off for days or even weeks before the first seizure. They noticed it but chalked it up to mood or the weather.
Common Causes of Seizures in Cats
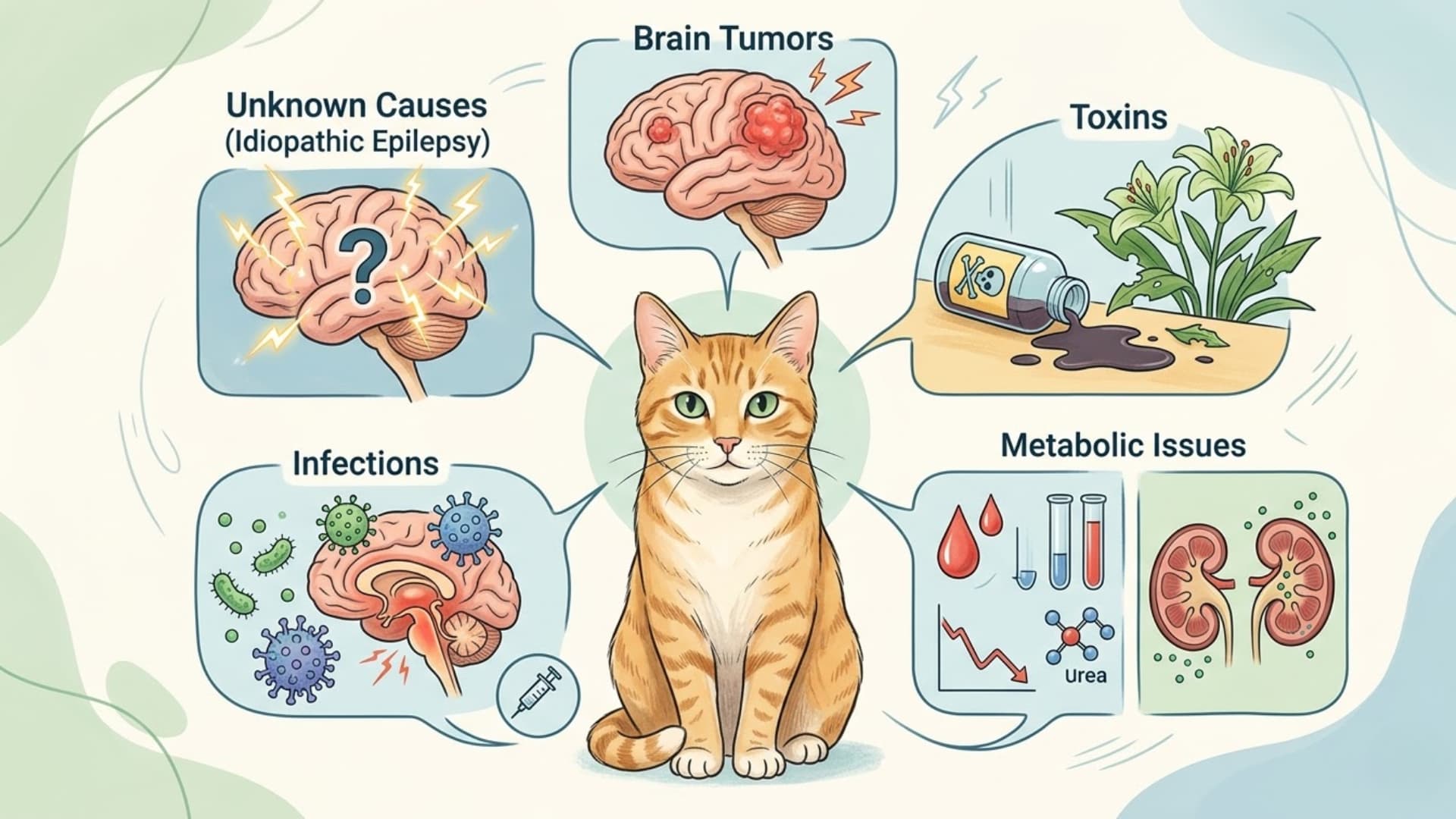
Seizures in cats can come from a range of underlying issues, some identifiable and treatable, while others remain unclear even after detailed testing and veterinary evaluation.
1. Idiopathic Epilepsy
In many cases, cats are diagnosed with idiopathic epilepsy, which means there is no identifiable reason behind the seizures.
Even after blood tests and scans, everything may appear normal. This can be frustrating for pet owners, but it is not uncommon.
The focus usually shifts to managing the seizures with medication and monitoring frequency, rather than finding a definitive cause.
2. Brain-Related Issues
Problems within the brain itself can trigger seizures. Tumors may grow and disrupt normal brain activity, especially in older cats.
Meningiomas are the most common brain tumor seen in senior cats and tend to grow slowly, which is why seizures in an older cat that was previously healthy should always prompt an MRI.
Depending on severity, treatment may include medication, surgery, or supportive care to manage symptoms.
3. Toxins and poisoning
Exposure to harmful substances is a common and often sudden cause of seizures in cats. This includes household chemicals, toxic plants, or certain human medications.
Permethrin toxicity deserves special attention; it is one of the most preventable causes of seizure emergencies in cats.
Permethrin is found in many flea and tick products formulated for dogs. When applied to a cat, even accidentally or in small amounts, it can cause severe, violent muscle twitching that is frequently mistaken for a seizure.
Symptoms usually appear without warning and may be severe. Immediate veterinary care is critical in these situations, as early treatment can sometimes reverse the effects.
If your household includes both a dog and a cat, switching to a natural flea and tick spray for dogs that does not contain permethrin removes one of the most preventable seizure triggers entirely.
4. Metabolic Problems
Internal imbalances in the body can also lead to seizures. Low blood sugar levels can deprive the brain of energy, while liver disease can cause toxin buildup in the bloodstream.
Both conditions interfere with normal brain function. These issues are often detected through blood tests and may be managed with medication, diet changes, or ongoing treatment plans.
5. Infections and Inflammatory Conditions
Certain infections can affect the brain and nervous system, leading to seizures. In younger cats specifically, Feline Infectious Peritonitis (FIP) and toxoplasmosis are notable infectious causes that can produce neurological symptoms, including seizures.
These are worth testing for in cats under five years old who present with seizures alongside other systemic signs like lethargy, weight loss, or fever.
These may include viral, bacterial, or parasitic infections. In some situations, even after thorough testing, no clear cause is found. Treatment then focuses on reducing seizure frequency and maintaining the cat’s quality of life.
Is It a Seizure, or a Cardiac Syncope?
This distinction matters more than most guides acknowledge. Cardiac syncope, fainting caused by a sudden drop in blood flow to the brain, can look remarkably similar to a seizure.
Both can cause a cat to collapse suddenly and become briefly unresponsive.
The key differences: during a true seizure, you will typically see rhythmic muscle paddling, leg jerking, and urinary or fecal incontinence, followed by a post-ictal confusion period.
During cardiac syncope, the episode tends to be shorter, the cat usually does not paddle or convulse, and they often recover quickly with no post-ictal disorientation.
If your cat has heart disease or an arrhythmia, mention this to your vet before assuming the episode was a seizure; the diagnostic and treatment path is entirely different.
What to Do When Your Cat Has a Seizure
When your cat has a seizure, staying calm is the most important thing you can do. Here is a clear, step-by-step approach:
- Do not restrain your cat or touch their mouth: Cats cannot swallow their tongue during a seizure. Putting your fingers near their mouth puts you at serious risk of a severe bite.
- Clear the space: Gently move nearby objects out of the way to prevent injury. If your cat is near stairs or furniture, guide them to a flat, safe surface if you can do so without physical contact.
- Dim the lights and reduce noise: Bright light and loud sounds can intensify the episode or distress your cat during the post-ictal recovery phase.
- Time of the seizure: Note when it starts. If your phone is nearby, begin a video recording; this footage becomes highly valuable for your vet’s diagnosis.
- Do not offer food or water immediately after: Cats are often disoriented after a seizure and can aspirate food or water during the recovery phase. Wait until they are fully alert and steady.
How are Cat Seizures Diagnosed and Treated?

Understanding how seizures are diagnosed and treated can help you feel more prepared, even though the process may involve ongoing care rather than a one-time solution.
1. Blood Tests and Imaging
When a cat has seizures, vets typically begin with blood tests to rule out metabolic issues like low blood sugar or liver problems.
These tests help identify underlying conditions that may be treatable. If results are unclear, imaging such as MRI or CT scans may be recommended to examine the brain for tumors, inflammation, or structural abnormalities that could be causing the seizures.
In some cases, your vet may recommend a cerebrospinal fluid (CSF) analysis, a procedure that examines the fluid surrounding the brain and spinal cord to detect infection or inflammation that standard imaging may miss.
2. Anti-Seizure Medications
The most common treatment for seizures in cats involves anti-seizure medications designed to reduce the frequency of episodes.
The two most frequently prescribed medications in cats are phenobarbital and levetiracetam (Keppra).
Phenobarbital has a longer history of use in veterinary medicine and is often the first-line choice, though it requires periodic liver monitoring.
Levetiracetam is increasingly favored because of its favorable side-effect profile, particularly in cats with pre-existing liver concerns.
Treatment plans are usually long-term and require regular monitoring. Dosages may need to be adjusted over time based on how the cat responds and whether side effects appear.
3. Start a Seizure Log from Day One
One of the most underused but high-value tools for managing a cat with seizures is a dedicated seizure diary.
After each episode, note the date, time, duration, which body parts were affected, any behavioral signs you noticed in the hours before, and how long the post-ictal recovery took.
Over weeks and months, this log becomes your vet’s most reliable data source for adjusting medications and identifying whether the condition is worsening.
Many owners keep a simple notes app on their phone. Consistency matters more than format.
Reality check: It is important to understand that seizures are not always curable, especially when no clear cause is found. In many cases, the goal shifts from curing the condition to managing it effectively. With proper care and monitoring, many cats can still live a reasonably good life despite ongoing seizures.
Living With a Cat That Has Seizures
Living with a cat that has seizures requires small but important adjustments.
- Creating safe spaces, like soft resting areas away from sharp edges, helps reduce injury risk during episodes.
- Avoiding triggers, such as sudden loud noises or stress, can also make a difference.
- Pay close attention to the post-ictal phase as well, the hours after a seizure, when your cat is disoriented or temporarily blind.
- During this period, keep them in a quiet, confined area away from stairs or furniture they could fall from. Speak in a calm, low voice, but avoid forcing contact.
- Many cats find comfort in familiar smells, so placing an unwashed item of your clothing nearby can help them reorient without overwhelming stimulation.
Keeping your cat gently engaged without overstimulating them is a real balancing act. Cat enrichment activities include low-stress ideas that work well for cats with chronic health conditions.
When to Consider Euthanasia for a Cat With Seizures?
This is the conversation I have in my clinic that no one wants to schedule, but almost everyone quietly needs.
It is not about giving up. It is about understanding what comfort means when medicine has reached its limits.
There is no single threshold that tells you when it is time. But there is a set of meaningful indicators and cats whose quality of life has crossed a line that medication and care can no longer hold.
What matters most is not how long your cat can live, but how well they are living each day.
If the good moments are fading and distress is becoming the norm, it is worth pausing and reassessing.
This decision is rarely sudden. It builds over time through small changes that are hard to ignore.
Having an honest conversation with your vet can help bring clarity when emotions make it difficult to see things clearly.
Signs that Seizures are No Longer Manageable
There comes a point where seizures shift from being controlled episodes to ongoing suffering, and recognizing these signs early can help you make clearer decisions.
- Cluster seizures are becoming routine: If your cat is experiencing multiple seizures within a 24-hour period, despite being on medication, and this is escalating the situation.
- Prolonged post-ictal suffering: When recovery from each seizure takes longer, involves more distress, including persistent blindness, aggression, or inability to stand, and your cat is spending more time in post-ictal confusion than in lucid, comfortable wakefulness, the balance has shifted.
- Loss of basic functions or identity: A cat who no longer recognizes you, has stopped grooming, is unwilling to eat, or has lost control of basic body functions consistently.
- Medication side effects outweigh the benefits: Some anti-seizure medications, such as phenobarbital in particular, can cause liver stress and loss of coordination over time.
- You are managing fear, not life: If your cat’s day-to-day existence is primarily characterized by hiding, pain, disorientation, and the anxiety of waiting for the next episode, and this has been the consistent state for weeks, that is not a life being lived.
Conclusion
Dealing with seizures in cats is never easy, but understanding what is happening makes a real difference.
From recognizing early signs to managing treatment and monitoring your cat’s quality of life, every step helps you better support your cat.
Knowing the difference between a focal twitch and a grand mal episode, understanding what the post-ictal phase looks like, and having a filming habit ready, these are not small things.
They are the tools that lead to faster diagnoses, better medication decisions, and fewer emergencies.
While some cases can be controlled, others may become harder over time, leading to difficult decisions.
Knowing when to keep going and when to consider letting go is not about giving up; it is about choosing comfort over prolonged suffering.
At the end of the day, your focus should be on your cat’s well-being, not just survival. Trust your observations, lean on your vet, and remember that care also means knowing when enough is enough.
Frequently Asked Questions
Can Cat Seizures Cause Brain Damage?
Prolonged or repeated seizures, particularly status epilepticus, can cause irreversible brain damage due to sustained abnormal electrical activity and oxygen deprivation. This is one of the primary reasons prompt treatment of cluster seizures and status epilepticus is critical.
How Long is Too Long for a Cat Seizure?
Any seizure lasting longer than 5 minutes is a medical emergency. Repeated seizures without recovery between them (status epilepticus) also require immediate veterinary care.
Will My Cat Need Medication After One Seizure?
Not necessarily. Many cats are monitored after a first seizure and only start anti-convulsant medication if seizures become frequent, prolonged, or severe.